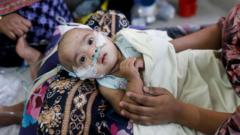
Why Bangladesh is seeing a deadly spike in measles
#Bangladesh #measles #outbreak #vaccination #childhood immunization #health crisis #infectious disease
📌 Key Takeaways
- Bangladesh is experiencing a significant increase in measles cases and deaths.
- The spike is attributed to a decline in routine childhood vaccination rates.
- Health systems are struggling to manage the outbreak amid other health challenges.
- Public health efforts are focusing on urgent vaccination campaigns to curb the spread.
📖 Full Retelling
🏷️ Themes
Public Health, Vaccination
📚 Related People & Topics

Bangladesh
Country in South Asia
Bangladesh, officially the People's Republic of Bangladesh, is a country in South Asia. It is the eighth-most populous country in the world and among the most densely populated with a population of over 171 million within an area of 148,460 square kilometres (57,320 sq mi). Bangladesh shares land bo...
Entity Intersection Graph
Connections for Bangladesh:
Mentioned Entities
Deep Analysis
Why It Matters
This measles outbreak in Bangladesh represents a significant public health crisis that threatens vulnerable populations, particularly children under five who face the highest mortality risk. The resurgence of a vaccine-preventable disease indicates failures in immunization systems and healthcare infrastructure, which could have ripple effects across South Asia. This outbreak affects not only families who lose children but also strains Bangladesh's healthcare system and could undermine decades of progress in child survival rates. International health organizations are concerned about potential spread to neighboring countries with similar vaccination gaps.
Context & Background
- Bangladesh had made significant progress in measles vaccination coverage through routine immunization programs over the past two decades
- The COVID-19 pandemic disrupted routine vaccination services globally, creating immunity gaps in many countries including Bangladesh
- Measles is one of the most contagious diseases known, with each infected person potentially spreading it to 12-18 others in unvaccinated populations
- Bangladesh achieved measles elimination status verification from the WHO in 2016 but has experienced periodic outbreaks since then
- The country faces challenges with healthcare access in remote areas and among Rohingya refugee populations
What Happens Next
Health authorities will likely launch emergency vaccination campaigns targeting affected regions and age groups within the next 2-4 weeks. International organizations like WHO and UNICEF will probably provide technical and logistical support for outbreak response. Bangladesh may need to reassess and strengthen its routine immunization systems to prevent future outbreaks, with potential policy changes announced within 3-6 months. The situation will be monitored for potential spread to neighboring countries like India and Myanmar.
Frequently Asked Questions
Measles is especially dangerous in Bangladesh due to high population density facilitating rapid spread, malnutrition weakening children's immune systems, and healthcare access challenges in rural areas. Children under five face mortality rates up to 10% in severe outbreaks when combined with complications like pneumonia or encephalitis.
Bangladesh's measles elimination status was undermined by COVID-19 disruptions to routine vaccination, leading to accumulating numbers of unvaccinated children. Declining vaccination rates over several years created sufficient susceptible populations for the virus to spread rapidly once introduced, despite previous elimination achievements.
Health authorities are implementing case detection and isolation, contact tracing, and preparing emergency vaccination campaigns in affected areas. Hospitals are establishing measles isolation wards and stocking treatments for complications while public awareness campaigns emphasize vaccination importance.
Yes, measles outbreaks can spread internationally through travel, particularly concerning given Bangladesh's connections with neighboring countries and diaspora communities. Countries with vaccination gaps are at risk, making this a regional public health concern requiring coordinated response.
Long-term solutions require strengthening routine immunization systems, addressing vaccine hesitancy through community engagement, improving healthcare access in remote areas, and establishing better disease surveillance. Sustainable funding and political commitment to immunization programs are essential for maintaining protection.